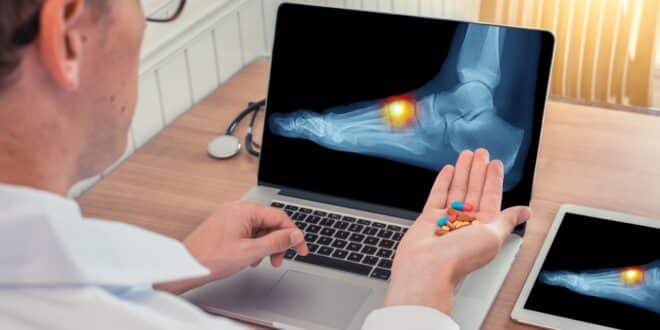
What is Rheumatoid Arthritis?
Our joints are usually made up of two bones that meet and are held together with tendons, cartilage, and muscle. A special tissue called synovium is within the joint area. This tissue produces a lubricant called synovial fluid that helps keep our joints moving.
Certain white blood cells from the immune system attack us in this disease. These cells induce swelling in the joint. The swelling causes the synovium to become thick, and it damages and/or destroys the cartilage and bones. This is why sufferers with arthritis experience warmth and redness in the area, weakness, and pain. Fingers and wrists are commonly affected. Other symptoms include anemia, neck pain, dry eyes, and in rare cases, inflamed blood vessels lining the lungs and/or the sac that holds the heart.
What causes Rheumatoid Arthritis?
Researchers are not too clear on the exact causes, but several areas may be considered.1
Genes. Researchers have identified several genes that are associated with rheumatoid arthritis. However, there are some people who have one or more of these genes, but they never get the disease. On the other hand, there are other people who do not have these genes, and they get the disease. More research needs to be done to help determine the role genes play in RA.
Environment. Researchers believe there are factors within our environment that increase our risk of the disease, but they are not clear on the culprit. They suspect a virus and/or bacteria infection might play a role. Research has not yet identified the exact agent.
Other Causes. More women are diagnosed with RA than men, and researchers suspect that hormones might play a role. For example, RA may flare up after pregnancy or during breastfeeding. In addition to hormones, other substances involved in swelling may play a role.
Arthritis Diagnosis and Treatment
Diagnosis of RA is somewhat difficult because there is no one test that doctors routinely use, and symptoms can differ from person to person. However, if there is a suspect of RA, check with the doctor to help diagnose the problem. Most likely, he or she will perform a medical examination, including blood tests. These tests may look for an antibody called rheumatoid factor and/or check the white blood cell count. Other tests may check for anemia and/or measure the C-reactive protein–this helps to determine the disease process in the body.
Treatments
Once a diagnosis has been established, your doctor may recommend one or more treatments.
Medication is one way to help prevent early damage, minimize or eliminate pain, and prevent or reduce inflammation. For example, analgesics help relieve pain, corticosteroids and nonsteroidal drugs help reduce inflammation, and disease-modifying antirheumatic drugs help to slow the disease process. Other drugs help to block certain white blood cells that cause inflammation, while others block body compounds that play a role in producing these white blood cells. Doctors can help make a choice on whether or not to use medications such as these.1
Lifestyle changes may also help ease symptoms and progression of the disease. If overweight, losing weight can help reduce the stress on the joints. It can also reduce body fat, reducing the production of inflammatory compounds. Moderate exercise helps with weight and overall health maintenance. Reducing stress helps to reduce the symptoms associated with RA.
Changes in the diet may help reduce symptoms and progression of the disease. Recently, researchers reviewed 15 studies involving 837 subjects and various diets. They reported that these studies might have some bias, but subjects reported reduced symptoms in one vegetarian and one Mediterranean study.2
Another article in Arthritis Today reported that in a test tube study, researchers found a higher count of antibodies in RA subjects who consumed cow’s milk, pork, codfish, cereal, hen’s eggs, and pork than in non-RA subjects. Researchers suggest the best way to determine whether or not a food increases antibody production is to go back to basics. Consume a plant-based diet that includes whole foods for a month and gradually add other foods to determine which one causes the symptoms.3
Foods That Help Decrease or Increase Inflammation
Several foods have been studied and show promise of symptom reduction.
• Omega-3 fatty acids have been studied for their role in helping to produce compounds in the body that reduce inflammation. Consuming about 3 grams of omega-3 fatty acids for more than 12 weeks showed reduced inflammation. Eating fatty fish such as tuna or salmon is rich in omega-3 fatty acids. Other foods, such as flaxseed and walnuts, contain a different form of omega-3 fatty acids called alpha-linolenic acid, which may also be helpful.
• Some omega-6 fatty acids may play a role in increasing inflammation. Increasing the omega-3 fatty acid intake and reducing the omega-6 fatty acid intake could help reduce inflammation. Reducing vegetable oil consumption, baked goods, and poultry can help lower omega-6 intake. 4, 5
• Gamma linolenic acid (GLA), another type of oil, may also help reduce inflammation. Evening primrose, borage, and black currant oils contain GLA. The research shows benefits from GLA, but the results are preliminary.
• Sweet Bing cherries provide several plant chemicals that may help reduce inflammation in some people. In one study, 18 healthy adults ate cherries for 28 days. Researchers reported that C-reactive protein and nitric oxide, two marker compounds for inflammation activity, were significantly reduced. 6
• Nightshade vegetables–potatoes, tomatoes, eggplant, and peppers contain a compound called solanine. This compound increases inflammation, and some people report that alleviating these foods from the diet reduces pain. However, research to support this is lacking.
• Herbal supplements are also used to find relief from symptoms, but the research lacks support for many of the herbs used. Some herbs are promising, and early research shows that there may be some benefits. Turmeric contains curcumin and may protect joints from inflammation and damage. Boswellia contains a resin that prevents inflammation activity in animal research. Human studies are still needed to confirm this action. Ginger contains anti-inflammatory compounds and may be shown to be beneficial.
If you liked this, you might also like Osteoarthritis Help
Pamela Williams writes from Southern California.
The John Hopkins Arthritis Center
1. Handout on Health: Rheumatoid Arthritis. 2009. http://www.niams.nih.gov/Health_info/Rheumatic_Disease/default.asp Accessed 3/18/2010.
2. Hagen KB, Byfuglien MG, Falzon L, et al. Dietary interventions for rheumatoid arthritis. Cochrane Database Syst Rev. 2009 Jan 21; (1): CD006400.
3. Mann DL. Rheumatoid Arthritis Diet: RA and Food Allergies. Arthritis Today. www.arthritistoday.org. Accessed 4/3/10
4. Calder PC. n–3 Polyunsaturated fatty acids, inflammation, and inflammatory diseases1,2,3. 2006. Am J Clin Nutr. Vol. 83, No. 6, S1505-1519S.
5. Kremer JM. N-3 fatty acid supplements in rheumatoid arthritis. Am J Clin Nutr. 2000;(suppl 1): 349S-351S.
6. Kelley DS, Rasooly R, Jacob RA, et al. Consumption of Bing sweet cherries lowers circulation concentrations of inflammation markers in healthy men and women. J Nutr. 2008;136:981-986.
7. Rheumatoid Arthritis and CAM. NCCAM, National Institutes of Health, U.S. Department of Health and Human Services. 2009.
© 2002 - 2025, AnswersForMe.org. All rights reserved. Click here for content usage information. Answers for Me Support & encouragement for every-day life
Answers for Me Support & encouragement for every-day life